For those with traumatic brain injury (TBI), aggression is a medical consequence, not a character flaw. The National Library of Medicine’s PubMed database documents aggression in up to 28% of severe TBI survivors within three months of injury, while research from the Model Systems Knowledge Translation Center notes that up to 75% experience significant irritability. Damage to the prefrontal cortex, which is the brain’s critical impulse regulator, is a primary driver of these behavioral changes.
New research offers a promising nutritional direction. A University of Pennsylvania meta-analysis, available on PubMed and re-amplified by ScienceAlert in May 2026, reviewed 28 randomized controlled trials with 3,918 participants and found omega-3* supplementation reduced aggression by up to 28%. Lead researcher Adrian Raine concluded, “I think the time has come to implement omega-3 supplementation to reduce aggression, irrespective of whether the setting is the community, the clinic, or the criminal justice system.”
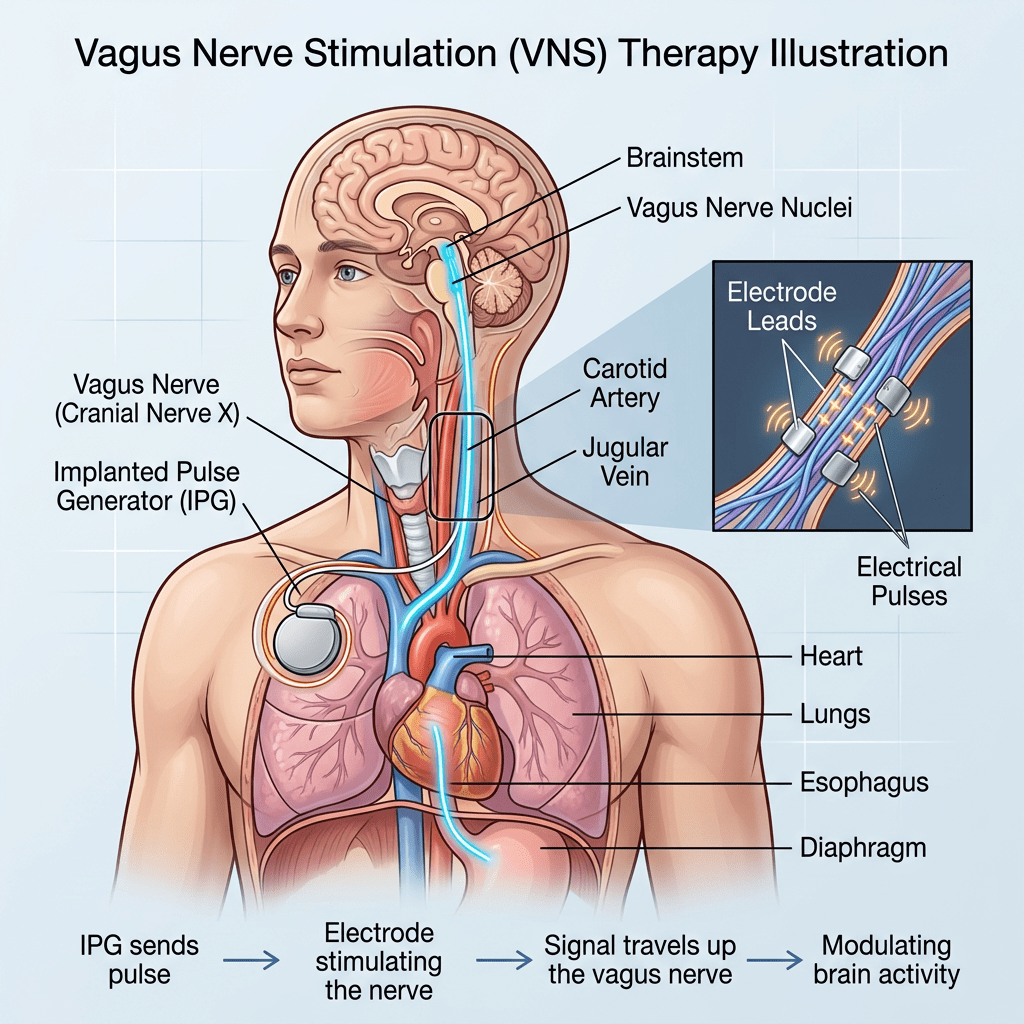
The biology is persuasive. DHA, the dominant omega-3 in brain tissue, concentrates in the prefrontal cortex – precisely the region TBI disrupts most – while EPA suppresses the neuroinflammatory cascade that worsens secondary injury. No TBI-specific clinical trial has yet directly targeted post-injury aggression as a primary outcome, but for survivors, omega-3 offers a low-risk, evidence-informed complement to existing care.
*Previous articles on TBIontheHill have noted additional benefits of Omega-3. Cherry-Picking Superfoods to Aid TBI Recovery (3/13/26) reported, “A cherry-chocolate brain smoothie is a good snack (tart cherries blended with cocoa powder, spinach, chia seeds, and almond milk) that delivers anthocyanins and omega-3s in one glass.” A Broader View of Diet’s Role in TBI Recovery (10/3/25) noted, “fruits, vegetables, healthy fats, and omega-3 fatty acids… These dietary interventions offer hope for… improving neurological outcomes without pharmaceutical interventions.”