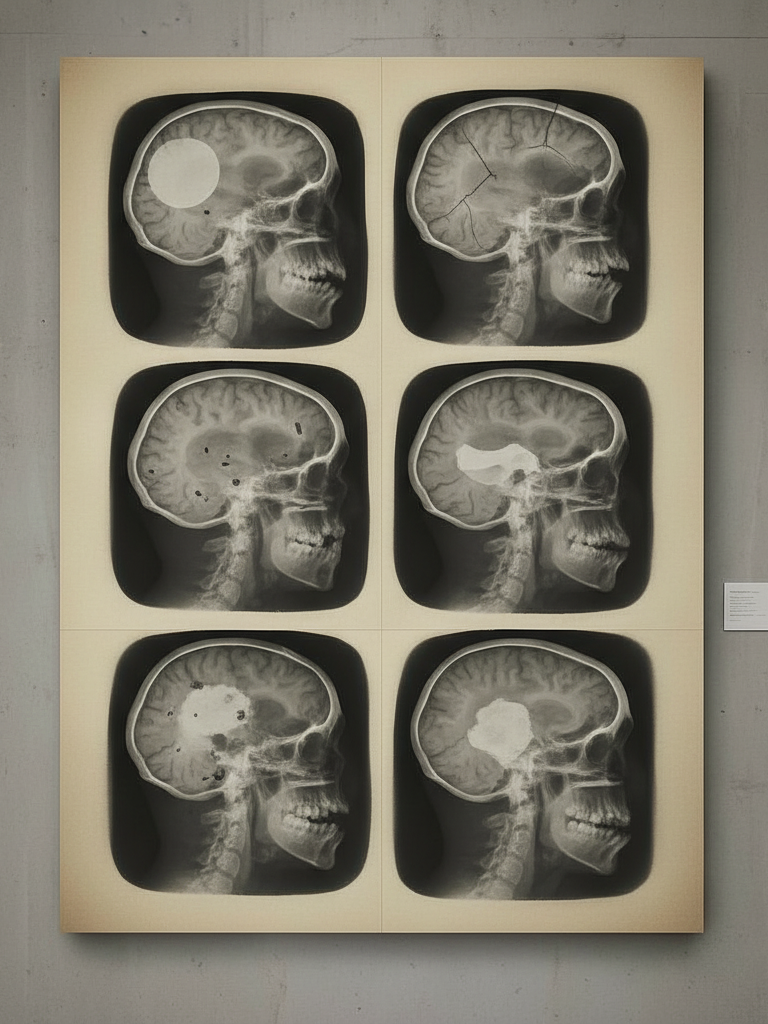
When a child arrives at an ICU with severe traumatic brain injury, every minute counts and every decision matters. That’s exactly the problem the Pediatric Guideline Adherence and Outcomes (PEGASUS) program was built to solve.
Developed in 2011 at the Harborview Medical Center, a Level I Trauma Center affiliated with the University of Washington School of Medicine, PEGASUS was created to close the so-called “know-do” gap, translating Brain Trauma Foundation guidelines into bedside practice. The program trains key staff, redesigns workflows, and provides ongoing coaching.
Published in Critical Care Medicine on March 27, 2026, a new study shows the model can reach far beyond Seattle. Across 16 hospitals in Argentina, Chile, and Paraguay, children with isolated severe traumatic brain injury at PEGASUS hospitals showed 8 percentage points higher guideline adherence than those receiving standard care. This determination came from the first randomized trial of an implementation science approach to improving care in adult or pediatric traumatic brain injury.
The reach of PEGASUS is backed by federal investment: the study was supported by a grant from the U.S. National Institute of Neurological Disorders and Stroke. As Dr. Monica Vavilala of UW Medicine clarified, this approach can be adopted by hospitals around the world, whether or not they are Level I Trauma Centers.