As any person who has given birth will confirm, pregnancy transforms nearly every system in the body. The brain is no exception to this change. Much of this neurological alteration is remarkably positive, but, as with other major body occurrences, some of it is genuinely alarming.
Estrogen and progesterone, which surges throughout pregnancy, are now being studied as neuroprotective and neuroregenerative agents in strokes and other brain injuries. Research shows these hormones can reduce the injury cascade by enhancing antioxidant mechanisms, reduce excitotoxicity, and stimulate remyelination. As researchers put it: “Estrogen seems more effective as a prophylactic treatment in females at risk for ischemic brain injury, whereas progesterone appears more helpful in post-injury treatment of both male and female subjects with acute traumatic brain damage.” Additionally, the 2022 Rotterdam Study, available on PubMed, examined 2,835 women over decades, finding that pregnancy and childbirth are associated with a robustly larger global gray matter volume that persists for decades.
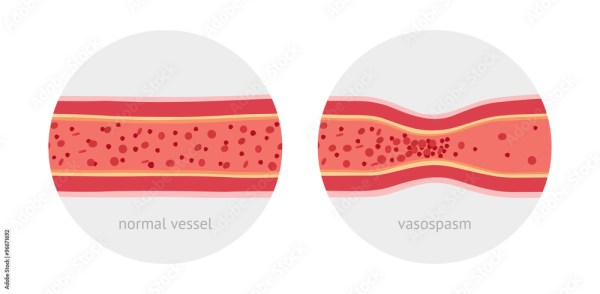
The story, though, isn’t all rosy. More recently, contradictory study results have been found. 2025 MRI research published in the International Journal of Molecular Sciences, found on PubMed, showed that pregnancy reduces total cortical gray matter volume by an average of 3%, with losses concentrated in regions linked to social cognition and self-awareness. More acutely, an estimated 7.7 – 15% of all maternal deaths worldwide are caused by stroke, and 30 – 50% of surviving women are left with persistent neurological deficits. “Female stroke survivors were more than twice as likely as their stroke-free counterparts to have another stroke while pregnant and in the six weeks after childbirth,” reported the 2026 American Stroke Association International Stroke Conference.
Ultimately, the pregnant brain endures, often emerging stronger. But, as with every activity that has a significant effect on the body’s function, proper monitoring is required, with even more caution needed for those with a history of brain injury.