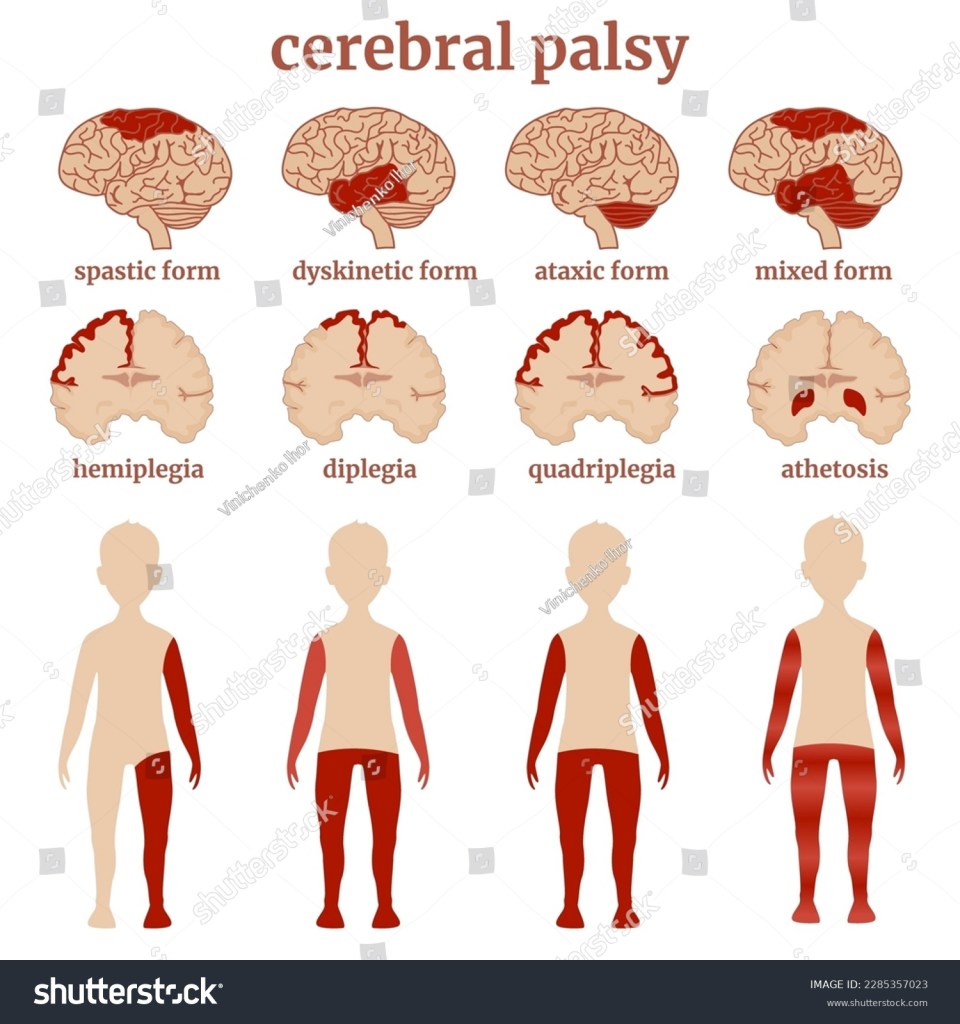
The brain injury comes first. Cerebral palsy follows. That distinction matters enormously, as CP is not itself a wound, but rather the permanent shadow one leaves behind.
The NIH’s National Institute of Neurological Disorders and Stroke guidance, reviewed as recently as March 13, 2026, describes CP as a disorder “caused by changes in the developing brain that disrupt its ability to control movement and maintain posture and balance.” The damage happens; CP is an outcome that the victim must live with in the future.
For most, the injury strikes before they ever draw a first breath. Oxygen deprivation during delivery, bleeding in the brain, or destruction of the delicate white matter surrounding a premature infant’s ventricles collectively account for roughly 80–90% of all cases. The CDC, in a February 2026 update, puts the scale in stark terms: about 1 in every 345 American children has CP, making it the most common childhood motor disability in the country.

Some cases, however, emerge after birth. Meningitis, near-drowning, and traumatic brain injury can all trigger CP, but only during the critical window when the brain is still forming, generally before age five. Once the skull has fully matured, the same injuries are referred to as traumatic brain injuries or acquired brain injuries.
To remedy what many see as the government’s chronic underfunding for CP, Tennessee Rep. Steve Cohen introduced H.R. 2178, Cerebral Palsy Research Program Authorization Act of 2025, on March 18, 2025. As he stated, “Cerebral palsy… is the most prevalent disability that has no designated federal funding for research.” After introduction, the bill was referred to the House Committee on Energy and Commerce. (No further action within the last Congressional session is reported.)

