The easiest way to heal from a brain injury is simply to replace the injured parts of the brain. Though this thought may seem both impossible and simply weird, scientists are now learning how to replace, or rather regrow, the brain in the healing of traumatic brain injury.
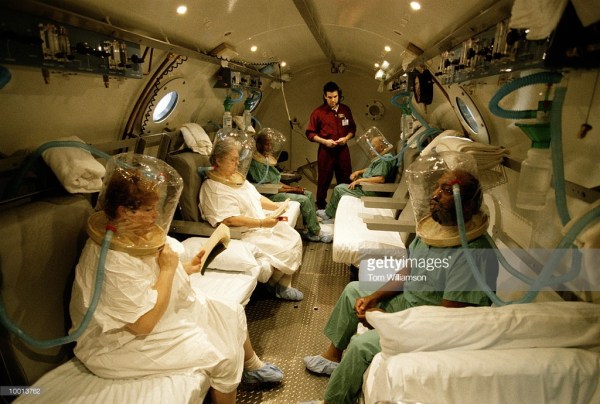
Specifically, it is well-known that human life depends of the inhalation of oxygen. Oxygen also helps the body heal, as it is transported through the body in red blood cells. Leveraging this healing process, hyperbaric oxygen therapy (HBOT) has been developed as a medical treatment in which one is encapsulated in a room or chamber filled with 100% oxygen. (The air humans typically inhale is only about 20% oxygen.) Additionally, HBOT has three times more air pressure than is typically experienced. Increased inhalation of oxygen means that it is not only transported through red blood cells, but also, “into all of the body’s fluids, the plasma, the central nervous system fluids, the lymph, and the bone.” More oxygen means more opportunities to aid healing, even while appropriate oxygen is still provided to the lungs.
Based on this evidence, it seems that HBOT would be a logical choice for professionals to treat those with certain injuries. For example, Lake Regional Wound Healing Center in Missouri has been named a Center of Distinction, largely for its work with HBOT.. In New Mexico, a pickleball benefit was recently held both to honor deceased veterans and to raise funds for Mission 22, an organization that offers HBOT to those with TBI.
More so, the federal government discovered these benefits a few years ago. In June 2014, for example, the NIH published a study titled Red blood cell transfusion in patients with traumatic brain injury: a systematic review protocol. In 2016, they published the results of a study titled Hyperbaric oxygen therapy for traumatic brain injury: bench-to-bedside, during which they concluded that, “HBOT has been demonstrated to have neuroprotective effects without increased oxygen toxicity in experimental TBI models when administered at pressures less than 3 ATA [atmospheric pressure].”
In recent days, a law to provide HBOT to veterans suffering from injury, including TBI and PTSD, was presented to the Arizona legislature. Specifically, Hyperbaric Oxygenation Treatment for Veterans with Traumatic Brain Injury was sponsored by Mark Finchem and passed the State House and Senate unanimously. On Thursday, March 29, HB 2513 was signed into law by Arizona Governor Doug Ducey. Reading about Arizona’s action reminds one that many other states have also passed such legislation: Oklahoma, Texas, Indiana and Kentucky.
* Two relevant questions regarding HBOT, with helpful answers:
“How does hyperbaric oxygen help brain injury or stroke? When cells in the brain die, either from trauma or lack of oxygen, blood plasma leaks out into surrounding brain tissue causing swelling and reducing blood flow. These otherwise normal cells go dormant because they can’t function without the appropriate amount of oxygen. HBOT dramatically increases the oxygen carried in the blood plasma, making oxygen available to heal damaged capillary walls, preventing plasma leakage and reducing swelling. As the swelling decreases, blood flow can be restored to the dormant tissue (neovascularization) and these cells then have the potential to function again.”
“How does hyperbaric oxygen help a child with cerebral palsy (CP) or traumatic brain injury (TBI)? In CP and TBI patients, some of the injured brain tissues may be “dormant” and non-functioning. HBOT can stimulate these “dormant” tissues and return them to more normal function. In young children, cognitive function and spasticity can be improved.”
